Polycystic Ovary Syndrome (PCOS) is widely recognized as a complex hormonal disorder that often disrupts menstrual cycles and complicates fertility in young adulthood. However, emerging research suggests a surprising silver lining: for many women, the condition may actually extend their reproductive window, delay menopause, and facilitate pregnancies later in life.
While PCOS presents significant challenges during a woman’s 20s and 30s, the physiological landscape shifts dramatically as she ages. Recent studies indicate that the very mechanisms that cause infertility in youth may resolve naturally over time, turning what was once a barrier into a potential advantage in the 40s and beyond.
A Finnish Study Reveals Delayed Menopause
The connection between PCOS and delayed menopause has been highlighted by research led by Terhi Piltonen at Oulu University Hospital in Finland. The study analyzed data from the Northern Finland Birth Cohort, tracking 1,849 women born in 1966 who underwent regular health checks throughout their lives.
At age 31, researchers identified 380 women who met the diagnostic criteria for PCOS. These women exhibited at least two of the following characteristics:
* Irregular or absent menstrual periods.
* Elevated testosterone levels.
* High levels of anti-Müllerian hormone (AMH), a marker produced by small ovarian follicles.
By age 46, the disparity in menopausal status was stark:
* Only 3% of women with PCOS had entered late perimenopause or menopause.
* In contrast, 18% of women without the condition had reached this stage.
This finding aligns with smaller studies, such as one conducted in Sweden, which found that women with PCOS typically reach menopause four years later on average than their peers.
Why “Crowded” Ovaries Change With Age
To understand why this shift occurs, it is necessary to look at the biology of the ovary. Piltonen and her colleagues suggest that women with PCOS are often born with a larger reserve of eggs.
The Youthful Challenge
In young adulthood, this abundance becomes a problem. The ovaries become “too tight” or crowded. When multiple eggs attempt to mature simultaneously, they often get stuck in mid-development due to this congestion.
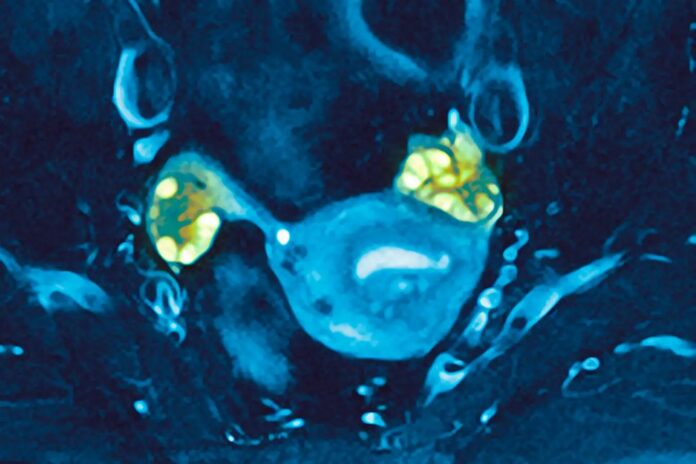
* These underdeveloped follicles appear as dark spots on ultrasounds.
* Historically, these were misidentified as cysts, leading to the misleading name “polycystic ovary syndrome.” (Note: Medical professionals are currently working to formally rename the condition to reflect this reality.)
* Because the eggs struggle to mature and release, ovulation is infrequent or absent, leading to irregular periods and reduced fertility.
The Later-Life Shift
As women age, the natural decline in egg count reduces this ovarian crowding.
* With fewer eggs competing for space, the remaining follicles can mature properly.
* Ovulation becomes more regular.
* Menstrual cycles stabilize.
“We call these children who they never thought they would have ‘evening stars’,” says Piltonen. Many women who struggled to conceive in their 30s are surprised to find themselves highly fertile in their 40s, often without the need for assisted reproductive technology (ART).
Health Implications and Evolutionary Context
The delayed onset of menopause associated with PCOS may offer significant health benefits. Menopause marks a sharp drop in estrogen, a hormone that protects against bone density loss, skin thinning, and heart disease. By delaying this transition, women with PCOS may enjoy prolonged protection against these age-related risks.
Research indicates that women who reach menopause after age 55 tend to live, on average, two years longer than those who enter menopause before age 40. This longevity suggests that the extended estrogen exposure provided by a larger egg reserve could be a protective factor for long-term health.
An Evolutionary Perspective
Piltonen proposes that PCOS may have offered evolutionary advantages to our ancestors. In environments where food was scarce and childbirth was risky, the traits associated with PCOS could have been beneficial:
* Energy Storage: A tendency to carry more weight provided a reserve during times of famine.
* Reproductive Resilience: The ability to reproduce at older ages ensured genetic continuity even if early-life fertility was compromised.
Given that PCOS is one of the most common endocrine disorders, its persistence in the human population suggests it likely conferred some survival benefit.
Conclusion
While Polycystic Ovary Syndrome remains a complex condition requiring management—particularly regarding metabolic health and early-life fertility—its impact is not uniformly negative. For many women, the condition acts as a biological buffer that delays menopause and extends the fertile window. Understanding this natural progression allows for better counseling and hope for women navigating fertility challenges in their later reproductive years.